Physician burnout is one of the most significant issues facing healthcare organizations today. A recent study by the Mayo Clinic found that the rate of burnout across all specialties is on the rise, up 46% from the three years previous1.
Although individual factors vary, it is widely accepted that increased documentation requirements and the use of EHRs have led to a dramatic increase in clerical activities, now accounting for twice as much time as clinical care1. This administrative burden is the largest contributor to physician stress, taking physicians away from what drew them to medicine in the first place - the care for patients.
Tools such as the AMA Mini Z Burnout Survey are helping hospitals understand and assess physician burnout and how this impacts hospital costs. Aside from direct costs to productivity and turnover, there is an established relationship between burnout and lower quality of care, decreased patient satisfaction and patient safety. Recent Mayo Clinic Proceedings show that the growing problem of burnout, technological dissatisfaction and administrative fatigue are leading one in fifty physicians to leave medicine within the next two years.
Understanding the Pillars of Physician Burnout
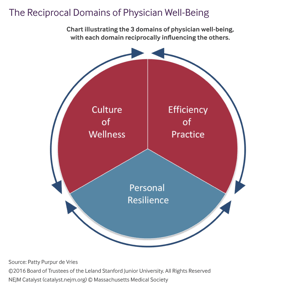
The Stanford Wellness Framework defines three reciprocal domains as the foundation for physician well-being: organizational culture, personal resilience and efficiency of practice (value-added clinical work accomplished). With this in mind, efficient communication between physicians, nurses, administrative and call center staff can have a significant impact on physicians’ well being.
Communication Tools Give Valuable Time Back to Physicians
At Telmediq, we’ve worked closely with CIOs, CTOs and physicians to solve critical inefficiencies in practice that are wasting valuable clinical time and leading to burnout, including:
- Support for team-based care - Support for threaded team messaging, with full archive of messages and results passed off during One-Click Safe Patient Handoff process or written back to the EMR
- Quick consultations - Easily look up specialists, by name or group, respecting call schedules. No need to reference the EMR, call schedules or contact clinics or call centers to support the connection
- Intelligent routing - Integrated on-call schedules and communication preferences mean doctors don’t get messages or alerts when they’re not available or on call
- Improved communication workflow with nurses - No more pager tag, calls or messages come directly to the physician with support for asynchronous two-way messaging
- Push results for critical labs - Critical lab results notify the care team, with no need to manually check the EMR
- Documentation support - Smart field mapping, user friendly design that writes directly back to the EMR supports real-time documentation. Auto-log critical lab receipts and chat threads back to the EMR to reduce documentation burden.
- One inbox for all messages - With indications for urgent messages or results
When implementing new technologies, the AMA suggests ensuring that one of the metrics for success includes clinician satisfaction and well-being. Contact one of our Clinical Communication Specialists today to learn more.
Sources: 1. Tethered to the EHR: Primary Care Physician Workload Assessment using EHR Event Log Data and Time-Motion Observations (Annals of Family Medicine, Vol 15, No 5 2017), Changes in Burnout and Satisfaction with Work-Life Balance in Physicians and the General US Working Population (Mayo Clinic, Published 2015), Professional Satisfaction and the Career Plans of US Physicians (Mayo Clinic, 2017)



